 Maybe even more interestingly, there appears to be significant plasticity of organization in the brain regarding the shift of language-eloquent hemisphere 5. However, right-hemispheric dominance may occur in roughly 4% of right-handed individuals and may be as high as 27% in extreme left-handers 5. This language-eloquent area is most often located in the left hemisphere, also in left-handed individuals 4. Superior division of the middle cerebral artery (MCA) It is bounded anteriorly by the ascending ramus of the lateral (Sylvian) fissure and posteriorly by the precentral sulcus. It is anterior to the primary motor cortex on the precentral gyrus. We recommend complete removal of these lesions to achieve a diagnosis and a permanent cure.Broca's area is located in the posterior inferior frontal gyrus ( pars opercularis (Brodmann area 45) and pars triangularis (Brodmann area 44)) of the dominant hemisphere, anterior to the anterior commissure line. Skull CH should be considered in the differential diagnosis of osseous tumors. Patients with brainstem CHs or poor neurological status face a higher risk for postoperative morbidity. Removal for CHs in eloquent regions may be considered on a case-to-case basis. Transient impairment may occur in up to one third of patients, but permanent morbidity is rare. The follow-up was in both cases uneventful.Ĭonclusion: In our experience in most patients CHs located in eloquent regions can be removed safely. The diagnosis of CH was histologically confirmed. Because of tumor progression it was decided to resect the affected bone en bloc. On the T1- and T2-weighted MR images the bone lesions were hypointense involving inner and outer table of the skull with and without enhancement after contrast administration. Each tumor had a diameter of 3,0 cm and was of a tender consistency. The skin over the skull lesions had a yellow appearance. An 8-month-old male infant had an additional CH arising from the right parietal skull. Both pediatric patients suffered from painless slow- growing bone lesions in the left frontal skull involving superior sagittal sinus. Adverse factors for the occurrence of surgical morbidity were pontine or brainstem location, smaller size of the CM, preoperative hemorrhage, poor neurological status and age. Postoperative improvement was correlated with good preoperative neurological status and younger age. 2 patients (6%) suffered severe permanent neurological deficit after surgery for a CM located in middle cerebellar peduncle and brainstem, respectively. 27 patients (81%) could live independently or recovered completely. According to the modified Rankin scale 13 patients (42%) had a slight (≥ 1 point) and 9 patients a moderate (≥ 2 points) impairment. Thirty patients (91%) had no new deficits or experienced improvement at the last follow- up. 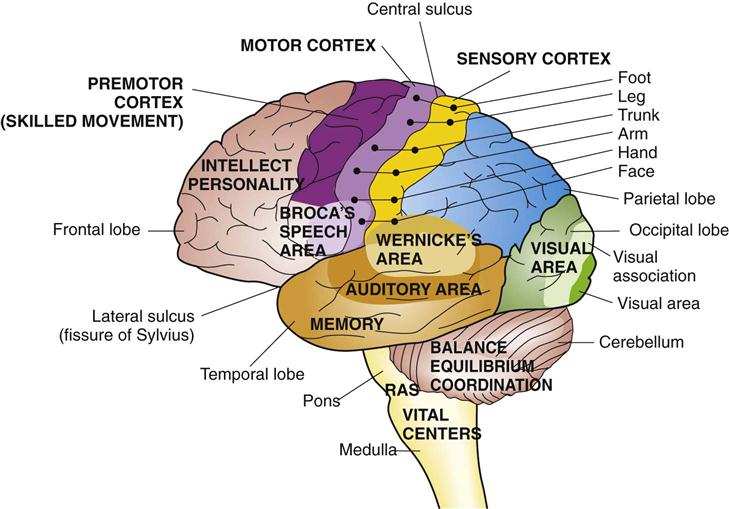
Neurological deterioration occurred immediately after surgery in 11 patients (27,5%). Results: Total resection was achieved in all patients with CH in eloquent regions without surgery-related mortality. Additionally, we analyzed the clinical and radiological signs, surgical approach and clinical course of the two pediatric patients. Outcome was evaluated using the modified Rankin scale. Long-term follow-up of the CHs was available in 33 patients (82,5%) with a follow-up to 80 months. The cerebral CHs were located in the following eloquent regions: sensorimotor system (n=13), brainstem (n=9), language areas (n=6), cerebellum (deep nuclei) and peduncles (n= 5), basal ganglia (n=5) and visual pathways (n=4). Methods: We reviewed the medical records and imaging studies of 40 patients (18 women and 22 men) with CHs in eloquent regions and of two 6- and 8-month old babies with solitary and multifocal congenital CHs of the skull, who underwent surgical resection. Here, we discuss two special situations: Cavernomas presenting as pediatric skull tumors and in eloquent regions. Objective: Cavernous hemangiomas (CH) are vascular malformations that usually can be operatively removed with a justifiable risk. This is an Open Access article distributed under the terms of the Creative Commons Attribution 4.0 License. Joint Meeting mit der Society of British Neurological Surgeons (SBNS).ĭüsseldorf: German Medical Science GMS Publishing House 2017. 
Jahrestagung der Deutschen Gesellschaft für Neurochirurgie (DGNC), 7. Society of British Neurological Surgeons.Ħ8. Medizinische Hochschule Hannover, Neurochirurgische Klinik, Klinik für Neurochirurgie, Hannover, Deutschlandĭeutsche Gesellschaft für Neurochirurgie. Klinikum Köln-Merheim, Klinik für Neurochirurgie, Köln, Deutschland Department of Neurosurgery, Hannover, Deutschland Medizinische Hochschule Hannover, Neurochirurgische Klinik, Hannover, Deutschland 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
